Piles: Causes, Symptoms, Stages and Best Treatment Options
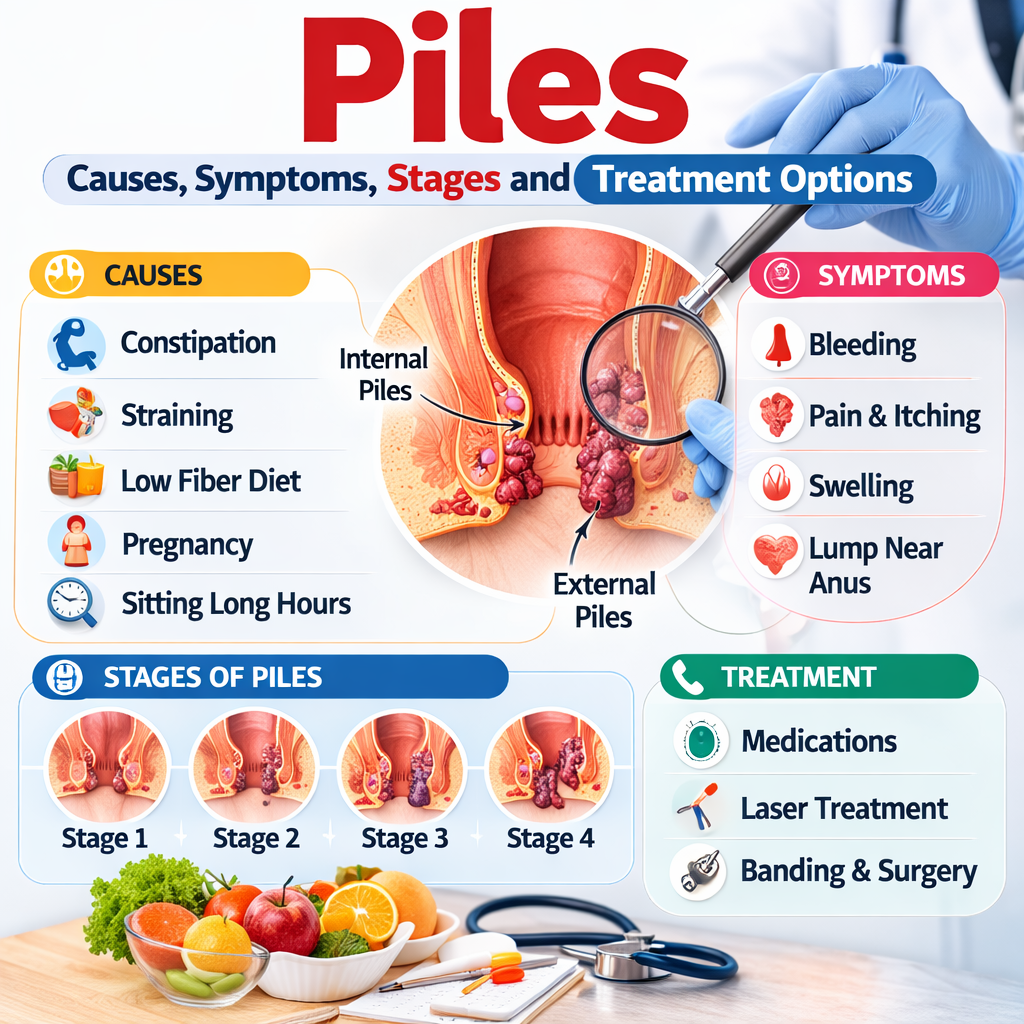
Piles, medically known as hemorrhoids, are among the most common conditions affecting the anal and rectal region. A large number of adults experience symptoms at some point in their lives, yet many people hesitate to discuss the problem due to embarrassment or lack of awareness. As a result, patients often ignore early warning signs such as bleeding during bowel movements, itching, or discomfort around the anus. Delayed medical attention may allow the condition to progress to more advanced stages that cause significant pain and complications.
Hemorrhoids develop when the veins in the lower rectum or anal canal become swollen due to increased pressure. This pressure can be caused by chronic constipation, excessive straining during bowel movements, prolonged sitting, pregnancy, obesity, or a low-fiber diet. Over time, the swollen veins enlarge and form hemorrhoids, which may lead to symptoms like bleeding piles, swelling around the anus, or difficulty sitting comfortably.
Understanding the causes, symptoms, stages, and treatment options for piles is important for early diagnosis and effective management. With modern medical care and lifestyle modifications, most patients can achieve long-term relief and prevent recurrence.
What Are Piles?
Piles are swollen and inflamed blood vessels in the lower rectum or around the anus. These veins normally function as vascular cushions that help maintain continence. However, when excessive pressure builds up in the rectal veins, the supporting tissues weaken and the veins enlarge, forming hemorrhoids.
Depending on their location and severity, hemorrhoids may cause symptoms such as rectal bleeding, itching, swelling, or pain during bowel movements. Some patients notice small lumps around the anus, while others experience painless bleeding during stool passage.
Piles are broadly categorized based on their location.
Types of piles include:
- Internal piles
- External piles
- Prolapsed piles
- Thrombosed piles
Internal piles occur inside the rectum and often cause painless bleeding. External piles develop under the skin around the anus and may cause pain, swelling, and irritation. In some cases, internal piles may protrude outside the anus and become prolapsed. When a blood clot forms inside a hemorrhoid, it results in thrombosed piles, which can cause sudden severe pain.
Causes of Piles
The development of piles is primarily related to increased pressure within the veins of the rectum and anal canal. When this pressure persists for long periods, the veins become enlarged and swollen, eventually forming hemorrhoids. Lifestyle habits and dietary patterns play a significant role in this process.
Constipation is one of the most common causes of piles. When stools are hard and difficult to pass, individuals tend to strain during bowel movements. This repeated straining increases pressure on the rectal veins and weakens the supporting tissues over time. Similarly, prolonged sitting—especially on the toilet—can impair blood circulation in the anal region and contribute to hemorrhoid formation.
Pregnancy is another important risk factor because the growing uterus increases pressure on the pelvic veins. Hormonal changes during pregnancy can also weaken vein walls, making hemorrhoids more likely to develop. Obesity and a sedentary lifestyle further increase the risk by placing additional pressure on the abdominal and rectal veins.
Dietary habits also play a crucial role. A diet low in fiber often leads to hard stools and irregular bowel movements, which increases the likelihood of straining and developing piles.
Common causes of piles include:
- Chronic constipation
- Straining during bowel movements
- Low-fiber diet
- Prolonged sitting or sedentary lifestyle
- Pregnancy and childbirth
- Obesity
- Aging and weakening of supporting tissues
These factors often act together, gradually increasing pressure on rectal veins and leading to hemorrhoids.
Symptoms of Piles
The symptoms of piles vary depending on the type and stage of the condition. In the early stages, patients may notice only mild discomfort or occasional bleeding. As the disease progresses, symptoms may become more noticeable and interfere with daily activities.
One of the earliest and most common symptoms of piles is bright red bleeding during bowel movements. This bleeding usually occurs without pain and may appear on toilet paper or in the toilet bowl. Many patients initially ignore this symptom, assuming it is temporary. However, persistent bleeding should always be evaluated by a medical professional.
Another common symptom is itching or irritation around the anus. This occurs because mucus discharge from hemorrhoids irritates the surrounding skin. Patients may also experience swelling or a feeling of fullness near the anal opening. In external piles, the swelling may be visible as a small lump that becomes painful when sitting or passing stool.
As hemorrhoids enlarge or prolapse, patients may develop discomfort during prolonged sitting and difficulty maintaining hygiene in the anal area.
Common symptoms of piles include:
- Bleeding during bowel movements
- Itching or irritation around the anus
- Pain or discomfort while sitting
- Swelling near the anal opening
- Lump around the anus
- Mucus discharge
The severity of symptoms often depends on the stage of the disease and whether complications such as thrombosis are present.
Stages of Piles
Internal hemorrhoids are classified into stages based on the degree of prolapse and severity of symptoms. This staging helps doctors determine the most appropriate treatment approach.
Stage 1 piles remain inside the anal canal and do not protrude outside. Patients may experience occasional bleeding but usually do not notice a visible lump. This stage is often managed with dietary changes and medications.
Stage 2 piles may protrude outside the anus during bowel movements but return inside spontaneously. Bleeding and mild discomfort may occur, particularly during straining.
Stage 3 piles prolapse outside the anus and require manual pushing to return inside. Patients often experience swelling, irritation, and recurrent bleeding.
Stage 4 piles remain permanently outside the anus and cannot be pushed back. This stage may cause severe pain, swelling, and complications such as thrombosis or ulceration.
Early recognition of these stages allows timely treatment and prevents progression to more severe disease.
Diagnosis of Piles
Diagnosis of piles usually begins with a detailed discussion of symptoms and medical history. A doctor evaluates factors such as bleeding during bowel movements, pain, itching, and swelling around the anus. Physical examination of the anal region helps identify external hemorrhoids and assess any visible swelling or inflammation.
Internal hemorrhoids may require additional evaluation using specialized instruments that allow visualization of the anal canal. These examinations are usually quick and minimally uncomfortable for patients.
Diagnostic methods commonly used include:
- Physical examination of the anal region
- Digital rectal examination
- Anoscopy or proctoscopy
- Colonoscopy in selected cases
These tests help confirm the diagnosis and rule out other conditions such as anal fissures, fistula, polyps, or colorectal disease that may present with similar symptoms.
Best Treatment Options for Piles
Treatment for piles depends on the stage of the disease and the severity of symptoms. Many patients can achieve significant relief through lifestyle modifications and medications, while others may require minimally invasive procedures or surgery.
Lifestyle management is the first step in treating early piles. Increasing fiber intake, drinking adequate water, and maintaining regular bowel habits can reduce constipation and prevent straining during bowel movements. Regular physical activity also improves digestion and promotes healthy bowel movements.
Medical therapy is often used to relieve symptoms such as pain, itching, and swelling. Stool softeners help make bowel movements easier, while anti-inflammatory medications and topical creams reduce irritation and discomfort.
For patients who do not respond to conservative treatment, minimally invasive procedures may be recommended. These treatments aim to shrink or remove the swollen hemorrhoidal tissue without major surgery.
Treatment options for piles include:
- Dietary and lifestyle modifications
- Medications and topical treatments
- Rubber band ligation
- Sclerotherapy
- Infrared coagulation
- Laser piles surgery
- Conventional hemorrhoid surgery
The choice of treatment depends on the stage of hemorrhoids and the overall health of the patient.
Laser Treatment for Piles
Laser treatment has become one of the most advanced methods for managing piles, particularly in moderate to advanced stages. This technique uses focused laser energy to shrink hemorrhoidal tissue while minimizing damage to surrounding structures.
Compared with traditional surgery, laser piles surgery is associated with less pain and faster recovery. Patients usually experience minimal bleeding during the procedure and can often return home the same day.
Advantages of laser treatment for piles include:
- Minimal pain after the procedure
- Reduced bleeding
- Short hospital stay
- Faster recovery
- Early return to daily activities
Because of these benefits, laser treatment has become a preferred option for many patients requiring surgical management of hemorrhoids.
Prevention of Piles
Preventing piles largely depends on maintaining healthy bowel habits and a balanced lifestyle. Diet plays a crucial role in preventing constipation and reducing strain during bowel movements.
Consuming fiber-rich foods such as fruits, vegetables, and whole grains helps soften stool and promotes regular bowel movements. Adequate hydration is equally important because water helps maintain proper stool consistency.
Regular exercise improves digestion and reduces pressure on abdominal and pelvic veins. Avoiding prolonged sitting, especially on the toilet, also helps prevent excessive strain on rectal veins.
Preventive measures include:
- Eating a high-fiber diet
- Drinking adequate water daily
- Exercising regularly
- Avoiding prolonged sitting
- Responding promptly to the urge to pass stool
- Maintaining a healthy body weight
Adopting these habits can significantly reduce the risk of developing hemorrhoids and prevent recurrence after treatment.
Conclusion
Piles are a common but often misunderstood condition that can significantly affect comfort and quality of life. Symptoms such as rectal bleeding, itching, or swelling around the anus should never be ignored, as they may indicate hemorrhoids or other anorectal conditions. Early recognition of the causes, symptoms, and stages of piles allows timely treatment and helps prevent complications.
With appropriate lifestyle changes, medical therapy, and modern procedures such as laser treatment for piles, most patients can achieve effective relief and return to normal daily activities. Seeking medical evaluation when symptoms first appear is the most important step toward safe and successful treatment.
